What are the Steps in the Medical Billing Process?
By: Valerie Smith, RN
Updated by: Michael Eugene | April 2026
Medical billing is a critical part of the healthcare revenue cycle. (New to the topic? Start with our introduction to medical billing and coding.) Medical billers are responsible for making sure that either insurance companies or patients pay healthcare providers for the services they deliver.
That process involves a specific series of steps from the moment a patient checks in to the final payment posting. Here’s how it works.
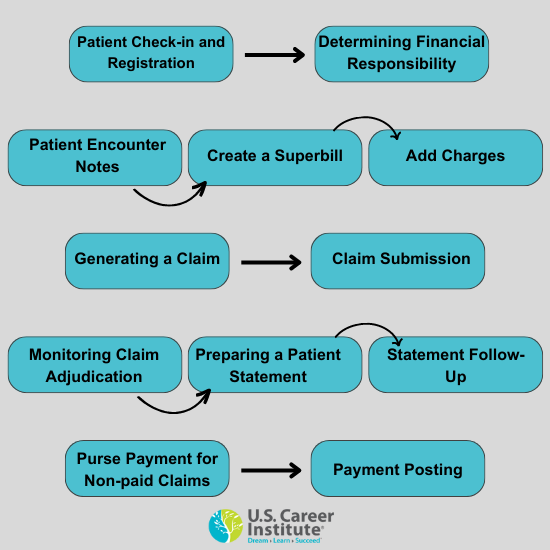
Patient Check-in and Registration
To begin, the patient will complete intake forms, or in the case of a return visit, they’ll review and update necessary information for the visit and insurance. The medical billing specialist will gather basic patient demographic information, including their name, date of birth, and the reason(s) for the visit.
Also, the medical billing specialist will identify the patient’s identification and collect the patient’s insurance information, including the insurer’s name and policy number. The medical biller verifies the accuracy and validity of the insurance information by contacting an insurance representative or entering the information into medical billing software. A patient file or medical record will initiate the medical billing process.
Determining Financial Responsibility
The medical billing specialist determines financial responsibility for the visit by identifying which medical procedures the insurance will cover. If the patient has secondary insurance, the medical billing specialist asks them to provide the insurance card and verify their coverage and benefits to identify if the secondary provider will pay the remainder of the bill. The medical billing specialist notifies the patient of any deductibles, co-pays, or balances due for procedures not covered by their insurance.
Patient Encounter Notes
During the patient’s visit, each healthcare provider must carefully note any treatments, diagnoses, prescriptions, and services rendered to submit medical claims accurately and receive payment.
Creating a Superbill
After the patient checks out, a medical coding specialist will translate the medical report into a diagnosis and procedure code (ICD, CPT, HCPCS, and modifiers) to create a superbill. The superbill will include the patient’s demographic information and medical history, procedure and service information, and the appropriate diagnosis and procedure codes.
Related: Learn more about exploring a career in medical coding and billing.
Add Charges
The medical billing specialist reviews the facility’s charges for the claim and aligns them with the appropriate medical billing codes to standardize medical services.
Generating a Claim
Using the information from the superbill, the medical billing specialist prepares a medical claim and submits it to the patient’s insurance provider. The medical billing specialist must review the claim to ensure it follows payer and HIPAA compliance standards.
Claim Submission
After reviewing the claim for accuracy and compliance, the medical billing specialist submits the claim. The medical billing specialist often submits the claim electronically to a clearinghouse. This is a third-party company that acts as a go-between for the healthcare provider and the insurance company.
This process is different for high-volume payers, such as Medicaid, as they often accept claims directly from healthcare providers. Some payers have specific guidelines for claim submission that medical billing specialists are required to follow closely.
Monitoring Claim Adjudication
Payers evaluate the medical claim and determine whether it is valid and compliant and the provider’s reimbursement amount through adjudication. The claim may be accepted, rejected, or denied.
The provider will receive payment according to the insurer’s agreements with an accepted claim. A rejected claim contains errors and requires correction before resubmission. The payer refuses to reimburse the provider if a claim is denied. The medical billing specialist must notify the patient of a denied claim and that they owe the provider the non-reimbursed amount.
If the patient has secondary insurance, the billing specialist can submit the remaining balance to that payer.
Preparing a Patient Statement
After processing the claim, the medical billing specialist bills the patient any outstanding charges not covered by insurance. The patient will receive a detailed statement explaining the procedures and services, costs, the amount the insurance paid, and the amount the patient owes the provider.
Statement Follow-up
The medical billing specialist ensures the healthcare facility receives payment for all claims or outstanding balances.
The medical billing specialist also follows up with patients who have delinquent accounts, providing them with details on a payment plan. This statement must include payment due dates and instructions on how the patient can pay their balance.
Pursue Payment for Non-paid Claims
The medical billing specialist monitors accounts receivable to identify when reimbursement claims are taking longer than expected. They also follow up with the patient for payment for denied claims.
Payment Posting
Finally, to close the process, the medical billing specialist posts payments to the patient’s account and deposits the received payment to the healthcare provider’s account.
Medical billing plays an essential role in the healthcare revenue cycle. A role in this field represents important, meaningful work. But did you know it can also be a rewarding, profitable, and exciting career . . . even for someone with little to no experience?
If you are interested in starting a new career journey as a medical billing specialist, a medical coding specialist, or potentially both in as little as 5 months, check out one of our certificate programs:
